Dental Implant Failure: Early Signs, Causes & What to Do

At Ufberg Dental, we work with patients every day who come in with questions about their dental implants. We have placed and restored implants for years, and we know how important it is to catch problems early. If something feels off with your implant, you deserve a clear, honest answer about what it might mean and what to do next.
This guide covers the early signs of dental implant failure, why implants fail, and the steps you should take if you notice a problem. If you are still researching whether dental implants are right for you, our implant page is a good place to start.
What Are the Early Signs of Dental Implant Failure?
Most dental implants are successful, but problems can happen. Knowing what to watch for can make a real difference in how things turn out.
Here is a quick overview of the main warning signs:
- Persistent or worsening pain beyond the first two weeks
- Swollen, red, or bleeding gums around the implant
- Any looseness or movement in the implant
- Pain or discomfort when chewing
- Gum tissue pulling back and exposing the implant post
- Pus, a bad taste, persistent bad breath, or fever
Each of these is covered in detail below.
Persistent or Worsening Pain
Some discomfort right after surgery is normal. What is not normal is pain that keeps getting worse after the first week or two, or pain that comes back months after your implant healed. If chewing or pressing on the implant causes sharp or aching pain, that is a sign something needs attention.
Swollen, Red, or Bleeding Gums
Mild swelling and bleeding can happen after implant surgery. But if your gums around the implant stay red, stay puffy, or bleed when you brush, that could point to an infection or early gum inflammation around the implant, sometimes called peri-implantitis.
Loose or Moving Dental Implant
A properly placed implant should feel like a natural tooth. It should not wiggle, shift, or feel unstable. Any movement of the implant is a warning sign and needs to be evaluated right away.
Pain or Difficulty When Chewing
Your implant is designed to handle normal chewing. If eating causes pain, pressure sensitivity, or discomfort, the implant may not have bonded properly with the jawbone, or there may be an infection developing.
Gum Recession Around the Implant
If the gum tissue around your implant starts to pull back, it can expose the metal post below. This can happen because of infection, bone loss, or improper placement. Recession does not fix itself on its own.
Pus, Bad Taste, Bad Breath, or Fever
These are signs of infection. Pus draining around the implant, a bitter or foul taste in your mouth, persistent bad breath, or a fever following implant surgery all require prompt dental attention. Do not wait to see if these symptoms go away.
Normal Healing vs. Dental Implant Failure Signs
Not every symptom after surgery means your implant is failing. Knowing the difference helps you stay calm and still take action when it matters.
Symptoms That Can Be Normal After Implant Surgery
In the first one to two weeks after surgery, it is common to have some swelling, bruising, mild bleeding, and tenderness at the implant site. These symptoms should gradually improve with each passing day. If you want a full breakdown of what pain to expect after surgery, see our guide on do dental implants hurt.
Symptoms That Should Not Be Ignored
Pain that gets worse instead of better, swelling that spreads, looseness in the implant, numbness that does not go away, and any sign of infection are not normal parts of healing. These symptoms always deserve a call to your dentist.
When Pain or Swelling Becomes a Concern
The general rule is this: if you are still experiencing significant pain or swelling two weeks after surgery, or if symptoms start to return after you felt fine, contact your dental office. Early action almost always leads to a better outcome. For more on typical pain timelines, read our post on how long dental implants hurt.
Why Dental Implants Can Fail
Understanding why implants fail helps you take steps to prevent problems and gives you context when something does go wrong.
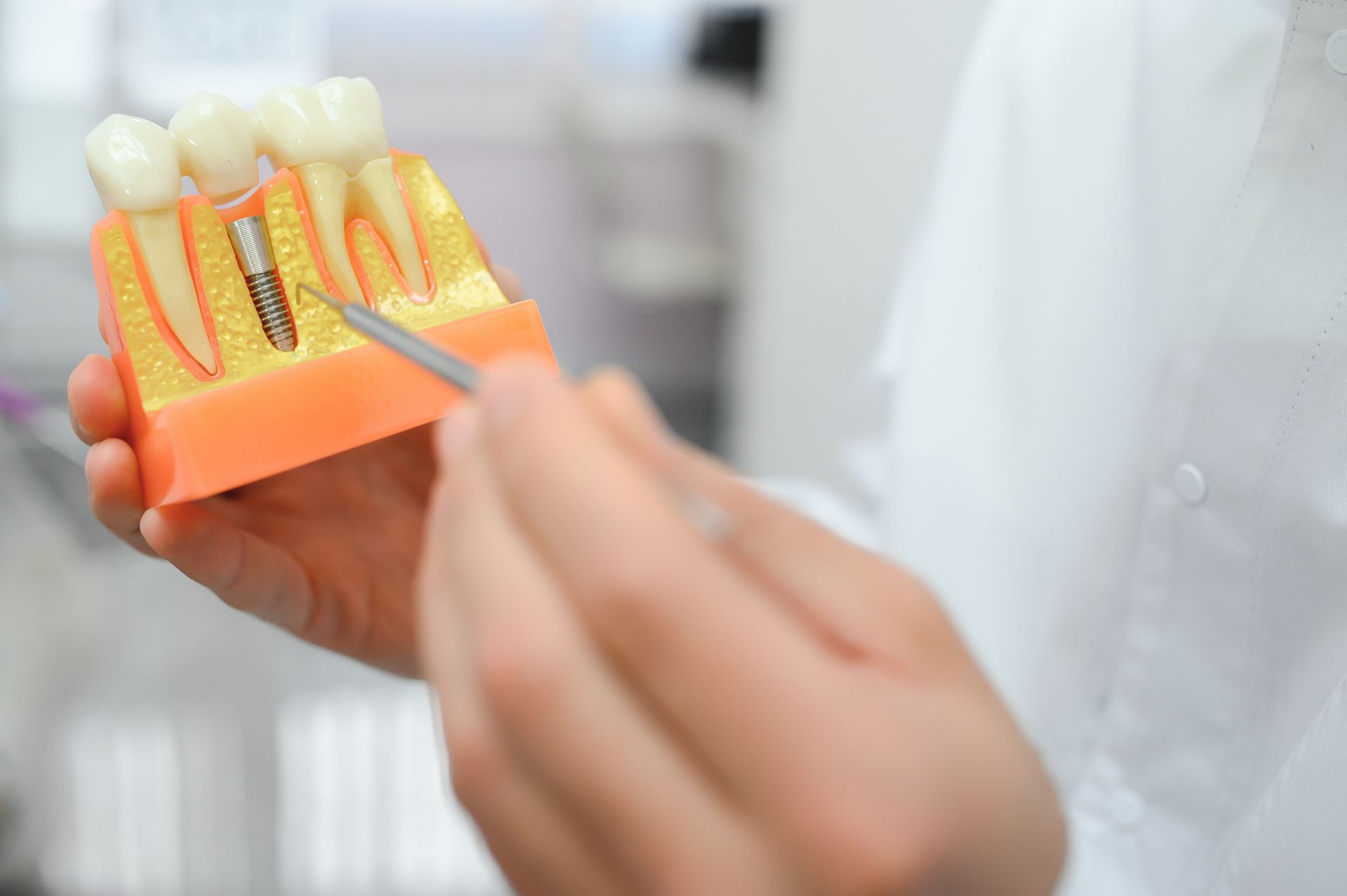
Poor Osseointegration
When the Implant Does Not Fuse Properly With the Jawbone
Osseointegration is the process where the implant post bonds with your jawbone. If this process does not complete successfully, the implant will feel unstable. Poor bone density, certain medications, or not following post-surgery care instructions can all affect how well osseointegration happens.
Peri-Implantitis and Infection
How Gum Inflammation Can Lead to Bone Loss
Peri-implantitis is a gum infection that affects the tissue and bone around the implant. It works similarly to gum disease around natural teeth. If left untreated, it causes the bone supporting the implant to break down, which can eventually lead to implant failure.
Bone Loss Around the Implant
Bone loss can happen for several reasons, including untreated infection, too much pressure on the implant, or a history of gum disease. When the bone around the implant shrinks, the implant loses its stable foundation.
Excessive Bite Pressure or Teeth Grinding
Bruxism, or grinding and clenching your teeth, puts significant force on dental implants. This repeated pressure can interfere with healing and cause the implant to loosen over time.
Smoking, Diabetes, and Other Health Risk Factors
Smoking reduces blood flow to the gums, which slows healing and raises the risk of infection. Uncontrolled diabetes also impairs healing. Patients with these risk factors need to be especially attentive to implant care and follow-up appointments.
Poor Oral Hygiene or Missed Dental Visits
Plaque that builds up around the implant can lead to infection. Skipping regular cleanings or checkups means that small problems do not get caught before they grow into larger ones.
Early vs. Late Dental Implant Failure
Implant failure can happen at different stages, and the cause and treatment often depend on when the problem starts.
| Early Failure | Late Failure | |
|---|---|---|
| When it happens | Within the first few months after surgery | Months or years after the implant healed |
| Main causes | Poor osseointegration, infection, healing complications, health conditions | Peri-implantitis, bone loss, teeth grinding, trauma |
| Common symptoms | Pain that does not improve, looseness, swelling that does not resolve | Gradual loosening, gum recession, returning pain, infection signs |
| Can it be saved? | Sometimes, with early treatment | Depends on severity; may require removal and replacement |
| Key takeaway | Act fast in the first weeks if healing feels wrong | Stay current on checkups even years after surgery |
Early Implant Failure After Surgery
Early failure happens within the first few months. It usually means the implant did not bond with the jawbone properly. Causes can include infection, bone issues, or healing problems related to health conditions or medications.
Late Implant Failure Months or Years Later
Late failure happens after the implant has already integrated with the bone. It is often caused by peri-implantitis, bone loss from infection, excessive bite pressure, or trauma. Late failures can sometimes develop slowly over a long period with minimal symptoms at first.
Why Timing Matters for Treatment
Knowing whether you are dealing with early or late failure helps your dentist choose the right treatment. In some cases, early intervention can save the implant. In others, the implant may need to be removed and replaced after the area heals.
What to Do If You Notice Dental Implant Failure Signs
If you notice any of the symptoms described above, the steps you take in the next few days matter.
- Call your dentist as soon as possible. Describe your symptoms so the office can prioritize your appointment.
- Avoid chewing on the implant side until you are seen. This reduces pressure on a potentially compromised implant.
- Do not try to adjust the implant yourself. Pushing or wiggling it can cause more damage to the surrounding bone and tissue.
- Expect an exam, X-rays, and a stability check at your appointment to get a clear picture of what is happening.
Call Your Dentist as Soon as Possible
Do not wait to see if the problem resolves on its own. Most dental offices can fit you in quickly when you describe symptoms of a possible implant problem. The sooner a problem is identified, the more options you have for treatment. If you are experiencing severe pain, swelling, or signs of infection, this may qualify as a dental emergency.
Avoid Chewing on the Implant Side
Until you are seen by your dentist, try to chew on the opposite side of your mouth. This limits added pressure on an implant that may already be compromised.
Do Not Try to Adjust the Implant Yourself
Never try to tighten, adjust, or push the implant back into place on your own. This can cause more damage to the bone and tissue around it.
Expect an Exam, X-Rays, and Stability Check
When you come in, your dentist will examine the implant site visually and take X-rays to check the bone levels around it. They will also check how stable the implant is. These steps give a clear picture of what is happening and what needs to be done.
Can a Failing Dental Implant Be Saved?
In some cases, yes. What is possible depends on how early the problem is caught and what is causing it.
Treatment for Infection or Gum Inflammation
If the problem is peri-implantitis or early infection, your dentist may prescribe antibiotics or antimicrobial rinses. Addressing the infection can stop further damage and, in some cases, allow the implant to stabilize.
Cleaning Around the Implant
A deep cleaning around the implant, similar to a periodontal cleaning for natural teeth, can remove bacteria and buildup that is contributing to bone loss and inflammation. This is often one of the first treatment steps.
Bone Grafting or Corrective Treatment
If bone loss has already occurred, a bone graft may be needed to rebuild the area. This can create a better environment for the implant to succeed long term or prepare the site for a replacement implant if needed.
When Implant Removal or Replacement May Be Needed
If the implant has failed completely, removal may be the best path forward. After the area heals, many patients are candidates for a replacement implant. Your dentist will explain your options based on your specific situation.
How to Reduce the Risk of Dental Implant Failure
Good habits before and after implant surgery go a long way toward keeping your implant healthy for years.
Keep the Implant Area Clean
Brush gently around the implant twice a day and floss or use an interdental brush daily. Keeping plaque away from the gum line is the single most important thing you can do to prevent infection.
Attend Regular Dental Checkups
Professional cleanings and checkups give your dentist the chance to spot early signs of trouble before you notice symptoms. Most patients with implants should come in every six months.
Treat Gum Disease Early
Active gum disease significantly raises the risk of implant failure. If you have gum disease, get it treated before getting an implant or, if you already have one, as soon as possible after diagnosis.
Wear a Night Guard If You Grind Your Teeth
If you grind or clench your teeth, a custom night guard can protect your implant from excessive force while you sleep. Ask your dentist if this is appropriate for you.
Avoid Smoking and Follow Post-Surgery Instructions
Smoking is one of the leading causes of implant failure. If you smoke, quitting before and after implant surgery greatly improves your odds of success. Follow your dentist's post-surgery instructions closely for the same reason.
Protect Your Dental Implant by Acting Early
Why Early Treatment Matters
Dental implants are built to last a lifetime with proper care. But like any dental restoration, they need attention when something goes wrong. Acting early almost always gives you more options and better outcomes than waiting until a problem becomes severe.
When to Schedule a Dental Implant Evaluation
If you have a dental implant and you are experiencing any pain, swelling, looseness, gum changes, or signs of infection, do not put off calling your dentist. Even if the symptoms turn out to be minor, getting checked gives you peace of mind and keeps small issues from becoming bigger ones.
Contact Ufberg Dental to schedule a dental implant evaluation and get the answers you need.
Frequently Asked Questions About Dental Implant Failure
How do I know if my dental implant is failing or just healing normally?
Normal healing involves gradually improving pain, swelling, and tenderness over the first one to two weeks. A failing implant is the opposite: symptoms that get worse instead of better, return after you felt fine, or never fully go away. Looseness in the implant at any stage is never normal. If you are unsure, call your dentist. It is always better to check and find nothing wrong than to wait on a real problem.
Can a failing dental implant be saved, or does it always need to be removed?
It depends on what is causing the failure and how early it is caught. Infections and early gum inflammation can often be treated with a deep cleaning, antibiotics, or antimicrobial therapy, and the implant can stabilize. If significant bone loss has already occurred, a bone graft may be needed. Complete failure where the implant has lost its bond with the bone typically requires removal, followed by a replacement once the area heals. Early action gives you the most options.
How long after implant surgery can failure still happen?
Implant failure can happen at two distinct stages. Early failure occurs within the first few months, usually because the implant did not bond properly with the jawbone. Late failure can happen years or even a decade later, most often due to peri-implantitis, bone loss, or excessive bite pressure. This is why regular checkups matter even after your implant has been stable for years.
Does a loose dental implant always mean it has failed?
Any looseness in a dental implant should be evaluated right away, but it does not always mean the implant is beyond saving. In some cases, a loose crown or abutment is the issue rather than the implant post itself. Your dentist will check whether the implant is truly mobile or whether the problem is with the restoration on top of it. Either way, do not ignore it or try to adjust it yourself.
What is the most common reason dental implants fail?
Peri-implantitis, a bacterial infection that causes inflammation and bone loss around the implant, is one of the most common causes of long-term implant failure. It develops when plaque is not consistently removed from around the implant, and it can progress without obvious symptoms in the early stages. Smoking, uncontrolled diabetes, and a history of gum disease all increase the risk. Regular cleanings and consistent oral hygiene at home are the most effective ways to prevent it.